March is Lymphedema Awareness Month, an opportunity to increase understanding of this often under recognised condition. Lymphedema is a chronic condition characterised by localised swelling, most commonly affecting the arms or legs, caused by a compromised lymphatic system. It may occur because of genetics or following surgery, lymph node removal, cancer treatment, infection or trauma. Without appropriate management, lymphedema can progress and increase the risk of complications such as recurrent infections.
In this article, our Vascular Specialist Nurse explains what lymphedema is, how it develops, and the treatment options available.

What is lymphedema and what are its symptoms?
Lymphedema is a condition of localized fluid retention and tissue swelling caused by a compromised lymphatic system. This results in swelling in one or more limbs. However, lymphedema can also occur in other body parts, e.g. neck, genital region, inguinal region, face, etc.
Here’s what you should know about lymphedema, its treatment, and why compression therapy is essential.
How do you recognize lymphedema?
- Swelling (called edema or congestion) in one or more limbs (often asymmetric)
- If lower extremity is involved, the swelling is present on the back of the foot
- Painless
- Feeling of tightness
- Restriction in range of motion, depending on lymphedema stage
- Thick or hardened skin, depending on lymphedema stage
- Recurring skin infections
- Stemmer’s sign positive, depending on lymphedema stage: This means that a fold of skin at the base of the second toe, the base of the middle finger, or another body part with swelling cannot be pinched and lifted.
What causes lymphedema?
Lymphedema is classified in two subtypes: primary lymphedema and secondary (or acquired) lymphedema.
- Hereditary: primary lymphedema is thought to be the result of a congenital abnormality of the lymph conducting system. It is estimated that primary lymphedema represents 5 to 10% of lymphedema cases.
- Acquired: secondary lymphedema results from damage to the lymphatic system (lymphatic vessels and/or lymph nodes) or from functional deficiency. Infections from insect bites, serious wounds, or burns can cause lymphedema when they damage or destroy the lymphatic system. Severe obesity, any type of surgery, serious injury, or radiation for cancer treatment (or the tumor itself) can cause the onset of the disease. Secondary lymphedema is thought to represent 90 to 95% of lymphedema cases.
The following factors can be causes of or lead to a progression or aggravation of existing lymphedema:
- Surgery (lymph node removal, e.g. cancer treatment)
- Trauma that might induce damage to the lymphatic system
- Radiation and chemotherapy as cancer treatment
- Serious infections of the skin or lymphatic channels (lymphangitis, cellulitis, erysipelas, microscopic parasite filarial larvae)
- Obesity
- Chronic venous insufficiency
Lymphedema has four stages:
Depending on disease progression, lymphedema can be divided into the following –
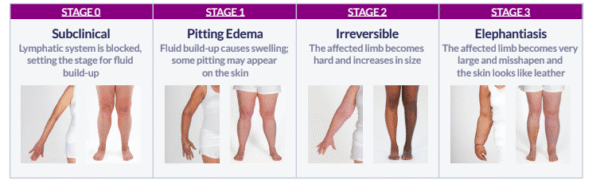
- In stage 0 (or Ia), swelling is not yet evident despite impaired lymph transport, subtle alterations in tissue fluid/composition, and changes in subjective symptoms. It may be months or years before overt edema occurs.
- In stage I, the accumulation of fluid subsides when you elevate the affected limb. When pressed by the fingertips, the affected area indents and reverses with elevation (“pitting”).
- Stage II signifies that limb elevation alone rarely reduces the tissue swelling. Pitting is manifest. Later in Stage II, the limb may not pit as excess subcutaneous fat and fibrosis develop.
- Stage III encompasses lymphostatic elephantiasis where pitting can be absent and trophic skin changes, such as acanthosis, alterations in skin character and thickness, further deposition of fat and fibrosis, and overgrowths have developed.
How can lymphedema be treated?
The “gold standard” and key treatment is CPD, this stands for Complex Physical Decongestive Therapy. CPD is based on two pillars
- Manual lymphatic drainage (Lymphatic Massage, offered at Bloom Skin Health, which is inside SVH, Willis St, Wellington). Gentle, specialized massage techniques designed to stimulate lymphatic flow. This is available from Bloom trained, senior therapists.
2. Medical Compression: Compression garments help maintain limb volume and prevent fluid re-accumulation. At SVH, our RN provides professional fitting for arm and leg compression garments, from Sigvaris.
Circular-knit compression hosiery is only used in the very early stages of lymphedema where the volume of the extremity has not yet reached extreme sizes. At SVH, this type of compression is available and fitted by our vascular registered nurse. We do not offer specialized treatments may be delivered by dedicated lymphedema clinics. In certain cases, we refer patients for custom flat-knit garments.
Skin Care
If the lymph flow is chronically disturbed, the protein-rich liquid accumulates in the soft tissue and the swollen body parts become inflamed. Also, the function of the immune system is reduced since the lymph system is impaired. Even a small injury to your arm or leg can be an entry point for infection (such as cellulitis or erysipelas) or severe inflammation.
Thus, it is important you maintain the integrity of your skin and carefully manage skin problems. This way, you minimize the risk of infections.
Recommended Skin care
- Washing daily, using pH neutral soap, natural soap, or a soap substitute
- If skin folds are present, ensuring they stay clean and dry
- Monitor the affected and unaffected skin for cuts, abrasions, and insect bites
- Applying emollients
- Avoiding scented products
Finally, we recommend exercises to help manage lymphedema
We recommend muscle pumping exercises, especially combined with external limb compression, performed daily, ie: walking, biking or climbing stairs.
If you notice persistent swelling in an arm or leg, early assessment is important. Lymphedema is a chronic condition, but with appropriate management it can be controlled and complications can be reduced. At SVH, we assess, diagnose and provide ongoing management plans tailored to each patient. Where specialized services are required, we can refer you to dedicated lymphedema providers to ensure comprehensive care. If you are concerned about swelling or would like advice regarding compression therapy, please contact our team for further information.